Neurologic Level Injury: The Definitive Guide to Understanding Your Spinal Classification
By Ellia Ciammaichella, DO, JD
Triple Board-Certified in Physical Medicine & Rehabilitation, Spinal Cord Injury Medicine, and Brain Injury Medicine
Quick Insights
Neurologic level injury refers to the lowest spinal segment with normal sensory and motor function after spinal cord damage. Doctors use standardized testing to map which nerve roots still work. This classification directly determines what movements and sensations remain possible. The neurologic level injury assessment helps predict long-term function and guides treatment planning. Accurate documentation matters because a difference of even one spinal level may impact independence potential.
Key Takeaways
- The ISNCSCI framework tests 10 muscle groups and 28 sensory points to classify injury severity.
- Complete injuries (AIS A) have no motor or sensory function below the injury level.
- Cervical injuries above C4 typically require ventilator support for breathing.
- Thoracic level injuries preserve arm function but affect trunk stability and leg movement.
Why It Matters
Understanding neurologic level injury classification helps attorneys evaluate medical records accurately and assess functional impact claims. This knowledge reveals whether expert opinions align with established clinical standards. It also clarifies why seemingly small differences in injury level produce dramatically different disability outcomes. Accurate classification directly affects case valuation and treatment cost projections in litigation contexts.
Introduction
As a board-certified physiatrist and attorney, I regularly evaluate spinal cord injury cases where understanding the neurologic level injury becomes critical for both medical and legal analysis. You can learn more about my dual expertise and approach by visiting the Ellia Ciammaichella, DO, JD biography page.
Neurologic level injury refers to the lowest spinal segment where both sensory and motor function remain normal on both sides of the body. This classification determines what movements a person can perform and what sensations they can feel after spinal cord damage. Accurate assessment of neurologic level injury directly shapes treatment planning, rehabilitation goals, and long-term functional expectations.
My dual training allows me to bridge clinical assessment with legal interpretation. I understand how small differences in documented injury level can dramatically affect independence potential and case valuation.
This article explains how physicians determine neurologic level injury using standardized frameworks and why this classification matters for evaluating medical records in litigation contexts.
What Is Neurologic Level in Spinal Cord Injury?
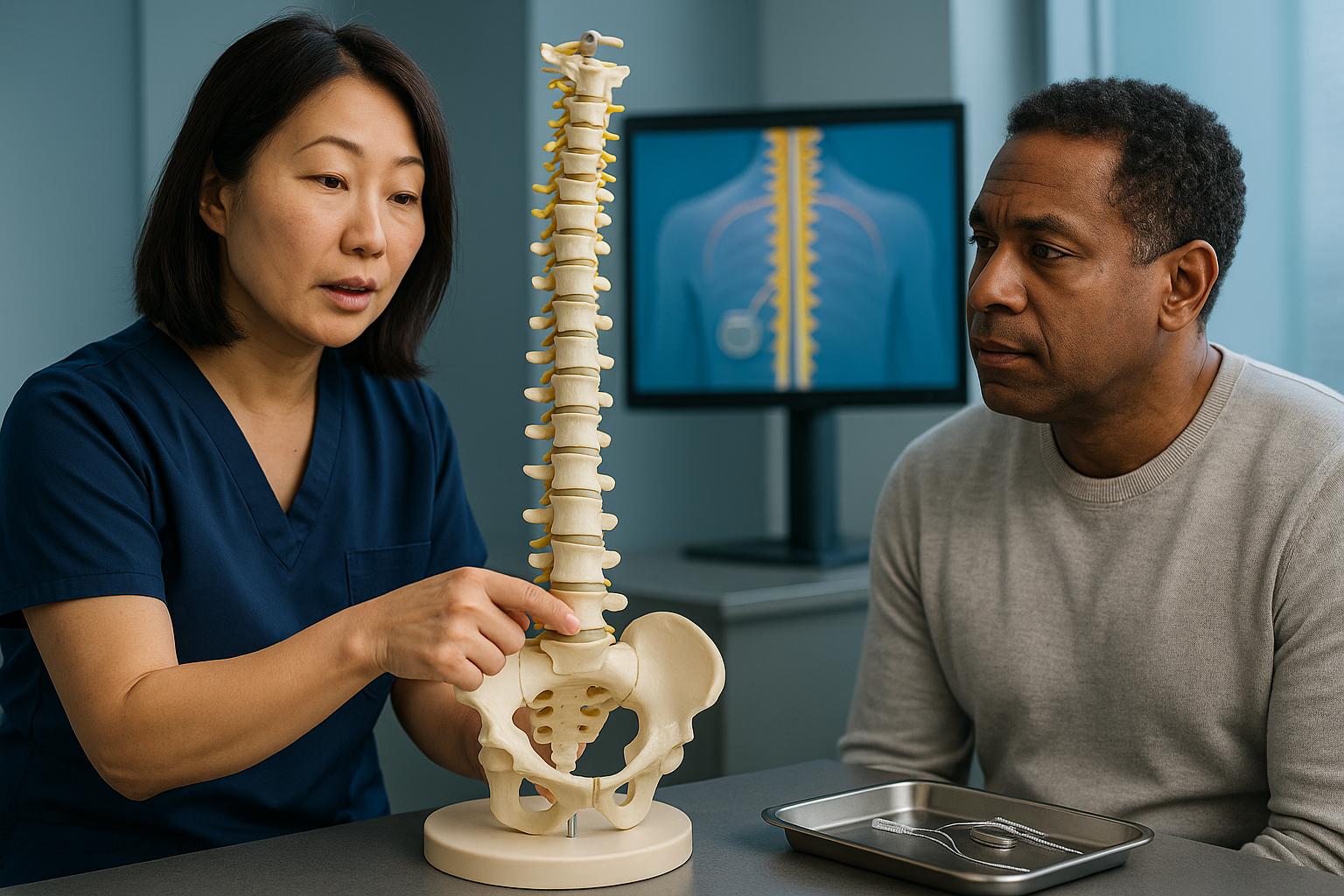
Neurologic level injury identifies the lowest spinal segment where both sensory and motor function remain intact on both sides of the body. This classification system helps physicians map exactly which nerve roots still work after spinal cord damage. The spinal cord comprises multiple segments, each contributing to the control of specific body regions and functions. When an injury occurs, everything below the damaged segment may lose normal function.
The neurologic level classification system provides a standardized way to describe injury severity and predict functional outcomes. I use this framework in every spinal cord injury evaluation because it directly determines what movements remain possible and what sensations a person can still feel. For example, a C6 neurologic level injury means normal function exists through the sixth cervical segment but not below it.
Understanding this classification matters because a difference of even one spinal level may impact independence potential. A C5 injury affects shoulder and elbow function differently from a C6 injury, which preserves wrist extension. These distinctions directly impact daily activities like eating, dressing, and wheelchair mobility.
If you’re interested in related discussions—such as how recovery milestones are evaluated after spinal cord injury—see how recovery milestones are evaluated after spinal cord injury.
How Doctors Determine Neurologic Level: The ISNCSCI Framework
Physicians use the International Standards for Neurological Classification of Spinal Cord Injury (ISNCSCI) to assess neurologic level injury. This standardized examination tests 10 key muscle groups and 28 sensory points on each side of the body. The testing follows a specific protocol that ensures consistency across different examiners and medical centers.
The 2019 ISNCSCI revision established current gold standards for classification and documentation. During the examination, I test muscle strength using a 0-5 grading scale for each key muscle group. Zero means no visible contraction, while five indicates normal strength against full resistance. For sensory testing, I assess light touch and pinprick sensation at specific dermatome locations.
The examination also identifies zones of partial preservation in complete injuries. This zone represents segments below the neurologic level where some sensory or motor function remains. The ISNCSCI framework has evolved through multiple revisions to improve reliability and clinical utility. Accurate documentation requires careful attention to testing technique and proper interpretation of borderline findings.
Attorneys and claims professionals seeking an in-depth understanding of medical-legal evaluation can learn about our medical-legal consulting services for expert witness testimony, IMEs, and case review.
Understanding the ASIA Impairment Scale (AIS)
The ASIA Impairment Scale classifies injury completeness using grades A through E. AIS A represents a complete injury with no motor or sensory function preserved in the lowest sacral segments. AIS B indicates incomplete injury with sensory but no motor function below the neurologic level.
AIS C means incomplete injury with motor function preserved below the neurologic level, but more than half of the key muscles below the level have strength grades less than three.
AIS D represents incomplete injury where at least half of key muscles below the neurologic level have strength grades of three or better. AIS E indicates normal sensory and motor function, though the person may have experienced spinal cord injury previously. Clinical case examples demonstrate how these classifications apply in real practice situations.
Distinguishing between AIS B and C requires careful motor testing below the neurological level of injury. The difference between AIS C and D depends on counting how many key muscles meet the grade three threshold. These distinctions matter because they correlate with different functional prognoses and rehabilitation potential.
How Injury Level Affects Daily Function
Cervical injuries above C4 typically require ventilator support because the diaphragm loses innervation. C5 injuries may preserve some shoulder and elbow flexion but can significantly affect hand function. Individuals with C5 injuries may be able to feed themselves using adaptive equipment but often require assistance with most other daily activities.
C6 injuries may preserve wrist extension, potentially improving independence. C6 injuries may enable tenodesis grip, where wrist extension facilitates passive finger flexion. C7 injuries may add elbow and finger extension, potentially enabling wheelchair propulsion and various self-care tasks. C8 injuries may preserve hand intrinsic muscles, potentially allowing fine motor control.
Thoracic level injuries preserve arm function but affect trunk stability and leg movement. Higher thoracic injuries compromise trunk balance and respiratory reserve. Lower thoracic and lumbar injuries preserve progressively more trunk control and may allow some leg function. Sacral injuries often preserve walking ability but affect bowel, bladder, and sexual function.
It’s important to recognize that functional correlation—how specific injury levels impact activities of daily living—can present unique challenges. For a closer look at transfers and independence strategies, see how transfers from wheelchair to bed are managed after SCI.
Why Accurate Classification Matters for Treatment and Prognosis
Accurate neurologic level classification guides treatment planning from the acute phase through long-term rehabilitation. Initial classification helps determine appropriate medical interventions, including surgical timing and approach. It also establishes baseline function for tracking recovery over time.
In rehabilitation settings, neurologic level determines realistic functional goals and necessary adaptive equipment. A C6 injury requires different wheelchair specifications than a C7 injury. Vocational planning depends heavily on preserved upper extremity function, which correlates directly with neurologic level.
Treatment selection for complications like neuropathic pain may also depend on injury characteristics. In medical-legal contexts, accurate classification affects disability ratings and life care planning costs. I frequently review cases where initial classification errors led to inappropriate treatment recommendations or inaccurate prognosis statements.
Documentation quality matters because the neurologic level can change during the acute and subacute phases. Serial examinations track neurologic recovery and help distinguish true improvement from initial examination errors. When reviewing medical records, I look for consistent documentation using standardized terminology and proper ISNCSCI scoring.
My Approach to Spinal Cord Injury Evaluation
Extensive experience in evaluating individuals with spinal cord and brain injuries has shown that accurate neurologic level classification serves as the foundation for every medical-legal analysis I conduct.
From my unique perspective with both medical and legal training, I understand how critical precise ISNCSCI documentation becomes in litigation contexts. A single spinal level difference can dramatically change disability ratings, life care planning costs, and functional prognosis statements. I’ve reviewed countless cases where initial classification errors led to inappropriate expert opinions or inaccurate damage assessments.
My dual credentials allow me to translate complex neurologic findings into clear documentation that serves both medical and legal needs. Whether working with defense teams requiring objective analysis or plaintiff attorneys seeking thorough functional assessment, I apply the same rigorous ISNCSCI standards to every evaluation.
Having extensive experience treating patients with spinal cord injuries, I’ve learned that standardized classification protects all parties by establishing objective baselines for tracking recovery and setting realistic expectations.
Conclusion
In summary, understanding neurologic level injury classification provides the foundation for evaluating spinal cord injury cases accurately. The ISNCSCI framework establishes objective standards that determine functional capacity, rehabilitation potential, and long-term care requirements.
As a physician and attorney, I’ve seen how precise neurologic level documentation directly affects case analysis and expert testimony credibility. Research demonstrates that accurate initial assessment shapes treatment decisions and prognosis statements throughout the recovery trajectory.
Based in Reno, Nevada, Dr. Ellia Ciammaichella provides medical-legal services through Ciammaichella Consulting Services, PLLC, across licensed states including Texas, California, and Colorado. I am available to travel for expert testimony and in-person evaluations when appropriate. This flexibility allows individuals and legal teams with complex cases to access consistent, expert analysis regardless of location.
I invite you to request a consultation today to discuss how a thorough neurologic level assessment can strengthen your case evaluation. Whether you need an objective medical record review or expert testimony regarding functional implications, my dual training ensures comprehensive analysis that serves both medical accuracy and legal clarity.
This article is for educational purposes only and should not be used as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified healthcare provider with any questions you may have regarding a medical condition or treatment options. Never disregard professional medical advice or delay in seeking it because of something you have read in this article.
Frequently Asked Questions
How does neurologic level injury differ from skeletal level injury?
Neurologic level injury identifies the lowest spinal segment with normal sensory and motor function on both sides of the body. Skeletal level refers to the vertebral location where bone damage occurred. These levels often differ because spinal cord segments don’t align perfectly with vertebrae.
A fracture at the T12 vertebra might produce an L1 neurologic level injury. This distinction matters because the neurologic level determines functional capacity, while the skeletal level indicates structural damage location. Medical-legal analysis requires understanding both classifications to evaluate causation and prognosis accurately.
Can the neurologic level change after the initial injury?
Neurologic level can change during the acute and subacute phases following spinal cord injury. Initial assessments may be limited by spinal shock, sedation, or other medical complications. Serial ISNCSCI examinations track recovery and distinguish true neurologic improvement from initial documentation errors.
Most neurologic recovery occurs within the first six months, though some patients show continued improvement up to two years post-injury. Accurate documentation of neurologic level changes affects disability ratings and life care planning costs in litigation contexts.
Why does a one spinal level difference significantly affect independence potential?
Each spinal segment controls specific muscle groups and body regions that determine functional capabilities. A C5 injury preserves shoulder and elbow flexion but lacks wrist extension, requiring significant assistance with daily activities. A C6 injury adds wrist extension, enabling tenodesis grip and dramatically improving independence with feeding, grooming, and wheelchair mobility.
This single-level difference changes equipment needs, caregiver requirements, and vocational potential. Understanding these functional correlations helps legal professionals evaluate expert opinions and assess damage claims accurately.
About the Author
Dr. Ellia Ciammaichella, DO, JD, is a triple board-certified physician specializing in Physical Medicine & Rehabilitation, Spinal Cord Injury Medicine, and Brain Injury Medicine. With dual degrees in medicine and law, she offers a rare, multidisciplinary perspective that bridges clinical care and medico-legal expertise. Dr. Ciammaichella helps individuals recover from spinal cord injuries, traumatic brain injuries, and strokes—supporting not just physical rehabilitation but also the emotional and cognitive challenges of life after neurological trauma. As a respected independent medical examiner (IME) and expert witness, she is known for thorough, ethical evaluations and clear, courtroom-ready testimony. Through her writing, she advocates for patient-centered care, disability equity, and informed decision-making in both medical and legal settings.
Medical Expert Services
Dr. Ciammaichella provides expert medical consulting for attorneys handling complex injury cases: